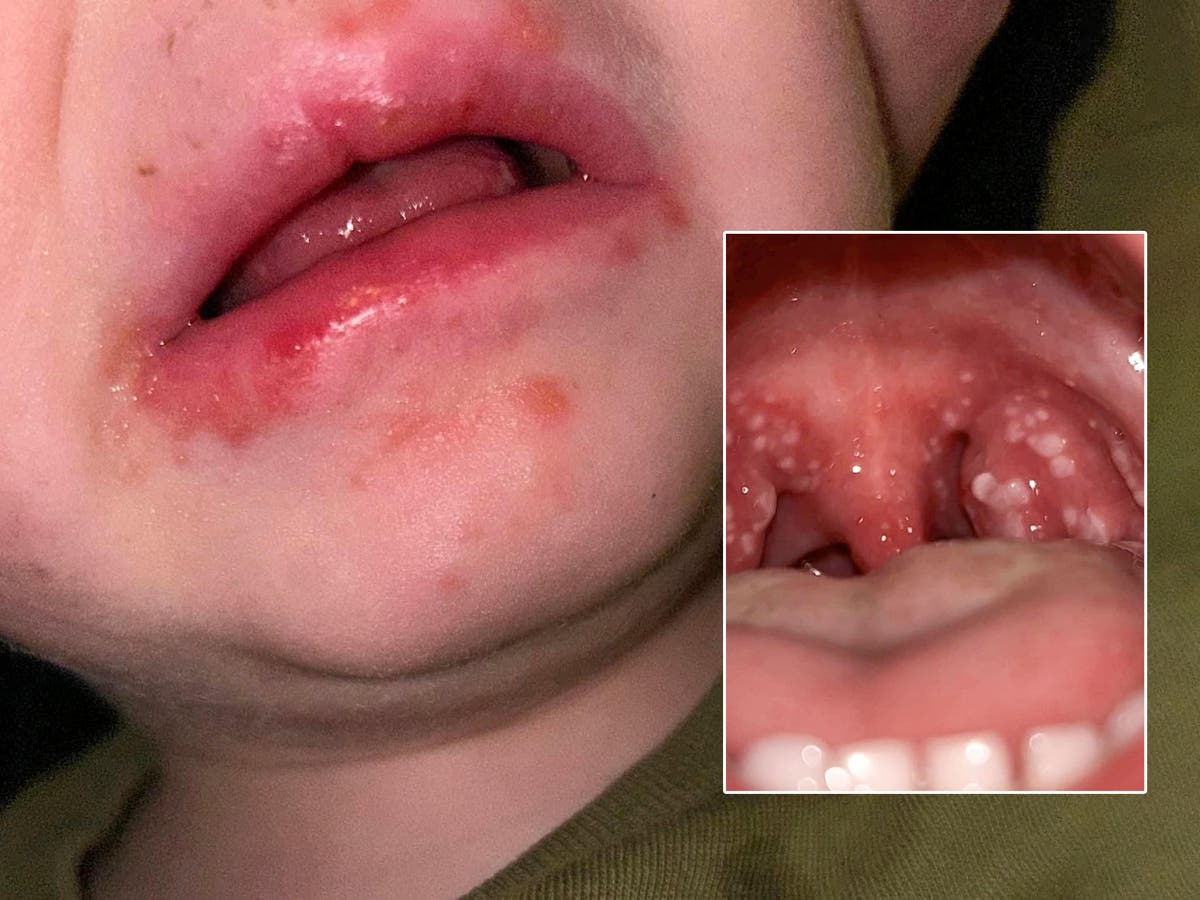
wCap started as a common bacterial infection that eventually killed 15 children in the UK who were infected with Strep A.
Health authorities have issued dire warnings for parents in the UK as the number of infant deaths due to infections continues to rise. The latest victim, a five-year-old Irish girl who became very ill last week, died on Monday of complications related to strep.
Although pediatric patients typically experience mild symptoms such as fever, swollen tonsils and lymph nodes, complications can arise when the infection enters the bloodstream, leading to a potentially fatal condition called invasive group A strep (iGAS).
In U.S., iGAS cases fall during pandemic, but CDC says independent On Wednesday, doctors in the United States notified the agency of a possible recent increase, which is being actively monitored.
Dr. Marc Heckar, a pediatric infectious disease specialist and associate professor in the Jacobs School of Medicine and Biomedical Sciences at the University at Buffalo, told independent It is difficult to know whether the United States will experience an outbreak similar to the recent outbreak in the United Kingdom.
According to data from the Centers for Disease Control and Prevention, before the outbreak in 2019, 7 children under the age of 17 died of streptococcal A complications per 100,000 people in the control area.
At the time of the last report, there was 1 death per 100,000 residents in controlled areas in 2020.
The CDC only tracks iGAs infections, not non-invasive Strep A infections. In the most recent report, only 10 countries reported iGAS data.
“Mitigation measures used during the first two years of the COVID-19 pandemic (eg, closing schools and workplaces, wearing face masks) helped limit the spread of many viruses and bacteria,” a spokesperson said.
“Now that these bacteria are circulating again, we may revert to the typical infection pattern of iGAS, including a seasonal increase in the winter months.
What is Strep A infection?
Group A strep infection is a common bacterial infection, mainly seen in children.
In more rare and more serious cases, infection can cause a pink rash (scarlet fever), bacterial dermatitis (impetigo), dead tissue (fasciitis), streptococcal toxic shock syndrome, pneumonia, and sepsis and other diseases.
However, most group A strep infections cause mild flu-like symptoms.
“There are many strains of group A strep and there have been isolated outbreaks in the UK in the past (2015 and 2018),” Dr Hekar said. “…with the pre-emergence surge in UK cases, there seems to be no impact on US cases, so [whether there will be one now] It’s hard to say. ”
Certain strains of infection can cause a “sandpaper rash,” which often makes children sicker more and is known as “scarlet fever,” Dr Hekar said.
This usually happens when [throat infections or] However, cases of pharyngitis can [happen with] The same is true for herpes infections. This appears to be the currently reported model in the UK.
Children with immunodeficiency are more likely to be infected with group A strep, he added.
“Some children with poorly functioning spleens or other forms of immunosuppression have an increased risk of sepsis, toxic shock, and necrotizing fasciitis (Group A carnivorous group),” Dr. Hekar said.
Doctors have warned the mother of 2-year-old Tayden, who was diagnosed with aplastic anemia earlier this year, that her daughter may delay her transplant after developing Strep A last week.
“She was exhausted the day before with a fever,” said Heather, who lives in Utah. independent.
Taiden’s symptoms disappeared within 48 hours of taking the antibiotic. You are expected to recover from transplant surgery.
Sore throat is one of the main symptoms of group A strep infection.
Will infection rates rise post-pandemic?
A CDC spokesperson said independent More data collection is needed to better understand recent trends in Strep A in the United States.
“The recent increase in respiratory viruses, particularly influenza, may lead to a potential increase in iGAS infection. Concurrent or previous viral infections, such as influenza, and skin diseases, such as chickenpox, may increase the risk of iGAS infection,” the spokesperson said.
Dr. Heka added that wearing a mask did not appear to reduce infections.
“Masks are good for treating respiratory viruses like flu and Covid, but other organisms that may linger on surfaces [such as Strep A] Mask use has not been affected to the same extent. “[US] From available data for 2020 (the first year of the pandemic), invasive group A infections and mortality appear to be stable. “
The CDC estimates that there have been 14,000 to 25,000 cases of iGAS over the past five years, with 1,500 to 2,300 deaths over the same period.
What symptoms should parents be aware of?
According to the CDC, most children infected with group A strep develop symptoms such as painful swallowing, fever, red and swollen tonsils (sometimes with white spots or streaks of pus), and swollen lymph nodes in the front of the neck.
Dr Heka says independent Sore throat and fever should go away within a few days. Parents are advised to contact their doctor again if symptoms persist.
If your child is diagnosed [Strep A] And it seems to get better, but then gets worse, discuss it with your doctor. “It could trigger one of these rarer and more serious complications.”
He emphasized that while most cases are not dangerous to children, complications can be fatal if the infection reaches the blood (bacteremia), lungs (pneumonia) or brain (meningitis).
New strain of group A strep may be more likely to cause serious internal infections
How are children infected?
Crowded places such as schools and day care centers increase the risk of Strep A infection.
The bacteria is highly contagious and can be spread through respiratory droplets produced when talking, coughing or sneezing, or by direct contact when sores appear on a patient’s skin, according to the CDC.
In rare cases, it can also spread through food if it’s not delivered properly.
“As social animals, we are constantly bombarded with bacteria and viruses that our immune system largely defends against,” Dr. Hekar said. independent.
“…more exposure [a person] The more likely they are to be infected. However, there are many benefits to peer interaction and socialization. ”
What should you do if you suspect your child has group A strep?
Strep A infection can be diagnosed with a rapid strep test that includes a throat swab.
Doctors also perform throat cultures on patients. This method, although it takes 1 to 2 days, is more effective than a rapid test.
What is the treatment for Strep A?
There is currently no vaccine to prevent Strep A infection.
Antibiotics, which reduce symptoms and prevent complications, are the most common form of treatment. Once antibiotics are prescribed, the patient should begin to feel better within 48 hours.