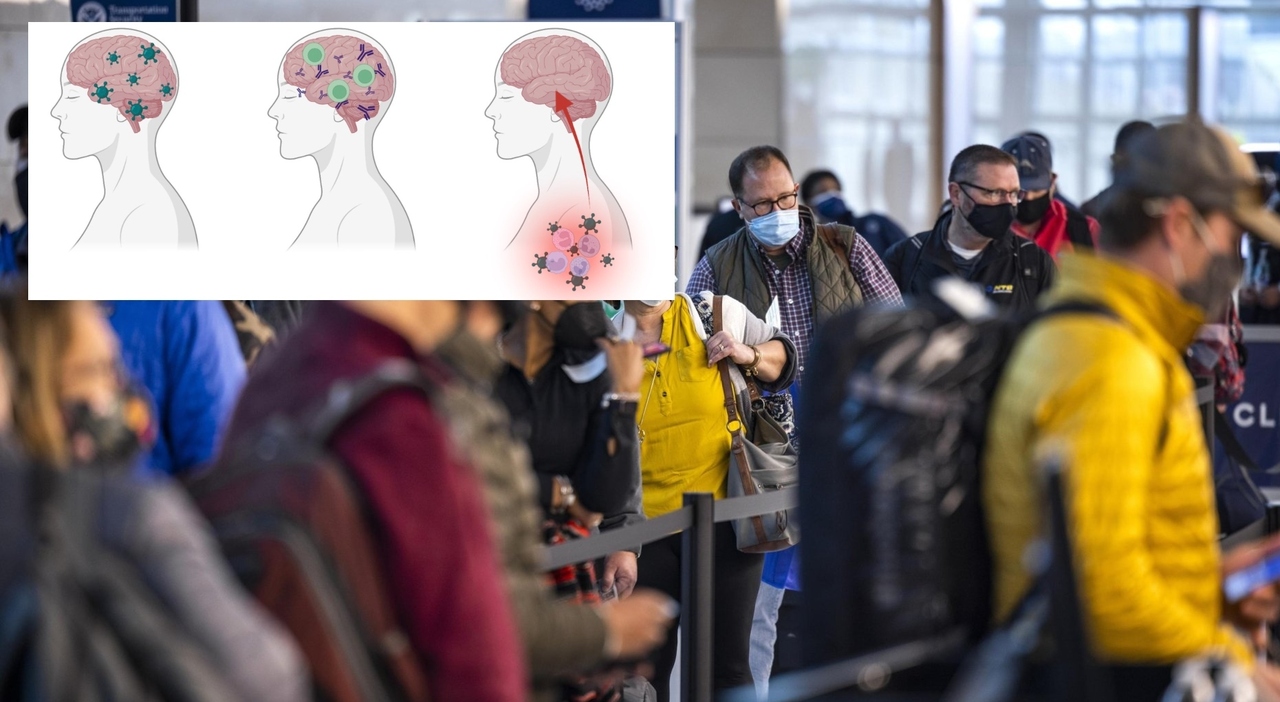
Lungs? No, maybe the brain. Recent international but also Italian studies are showing that in many medium-severe cases of infection with Covid-19, the virus after attacking the lungs and causing respiratory and matabolia problems, “settles” in the brain. The result at this point seems to be clear: it comes altered volume of some parts of the main human organ. Hence both neurological and psychiatric difficulties. Furthermore, according to studies, in patients hospitalized for a long time, particularly in intensive care wards, the lack of contacts with other social networks also contributes to reducing gray matter. A phenomenon recorded above all in young patients and in those of more advanced age in which there is a worsening of the ability to understand.
Omicron or Delta, which variant has infected ICU patients? The “tail” effect that engulfs hospitals
Long Covid: learning, sleep and mood disorders
According to Professor Akiko Iwasaki who works for the Cold Sprimg Harbor Laboratory, a private non-profit research center operating a few kilometers from New York, the loss is recorded seven days after the outbreak of a serious infection from Covid-19. of a third of the oligodentrocytes in some areas of the brain and the decline can last up to 7 weeks. What are oligodentrocytes? Particular cells that assist the functions of neurons in the central nervous system. Hence the behavioral and learning disorders but also sleep and mood disorders that were recorded in 70% of patients who were hospitalized in intensive care.
Furthermore, according to a study by the University of Brescia, up to 70% of patients with medium-severe disease resulting from SARS CoV-2 report neurological symptoms six months later, including chronic fatigue (34%), concentration (32%), sleep disturbances (31%), muscle aches (30%) and depression and anxiety (27%).
© breaking latest news
.